I spent years thinking my problem was Parkinson’s.
Turns out, part of the problem was how we were delivering the treatment.
Levodopa works. That is not the debate.
It is still the most effective tool we have for managing Parkinson's Disease.
But if the drug works, why does everything get harder over time?
The default answer is progression.
Neurodegeneration.
Loss of dopamine neurons.
All true.
But I do not think that is the whole story.
What We Know (and Keep Focusing On)
Levodopa does not just walk into the brain.
It has to cross the blood-brain barrier using the same transporter as large neutral amino acids. That means protein in the bloodstream can compete with it for entry.
That is real.
That matters.
It is why people talk about timing protein intake, spacing meals, and adjusting dosing schedules.
It is good advice.
But it is only part of the picture.
What We Built (and Do Not Question Enough)
Before levodopa ever gets to the blood-brain barrier, it has to survive everything leading up to it.
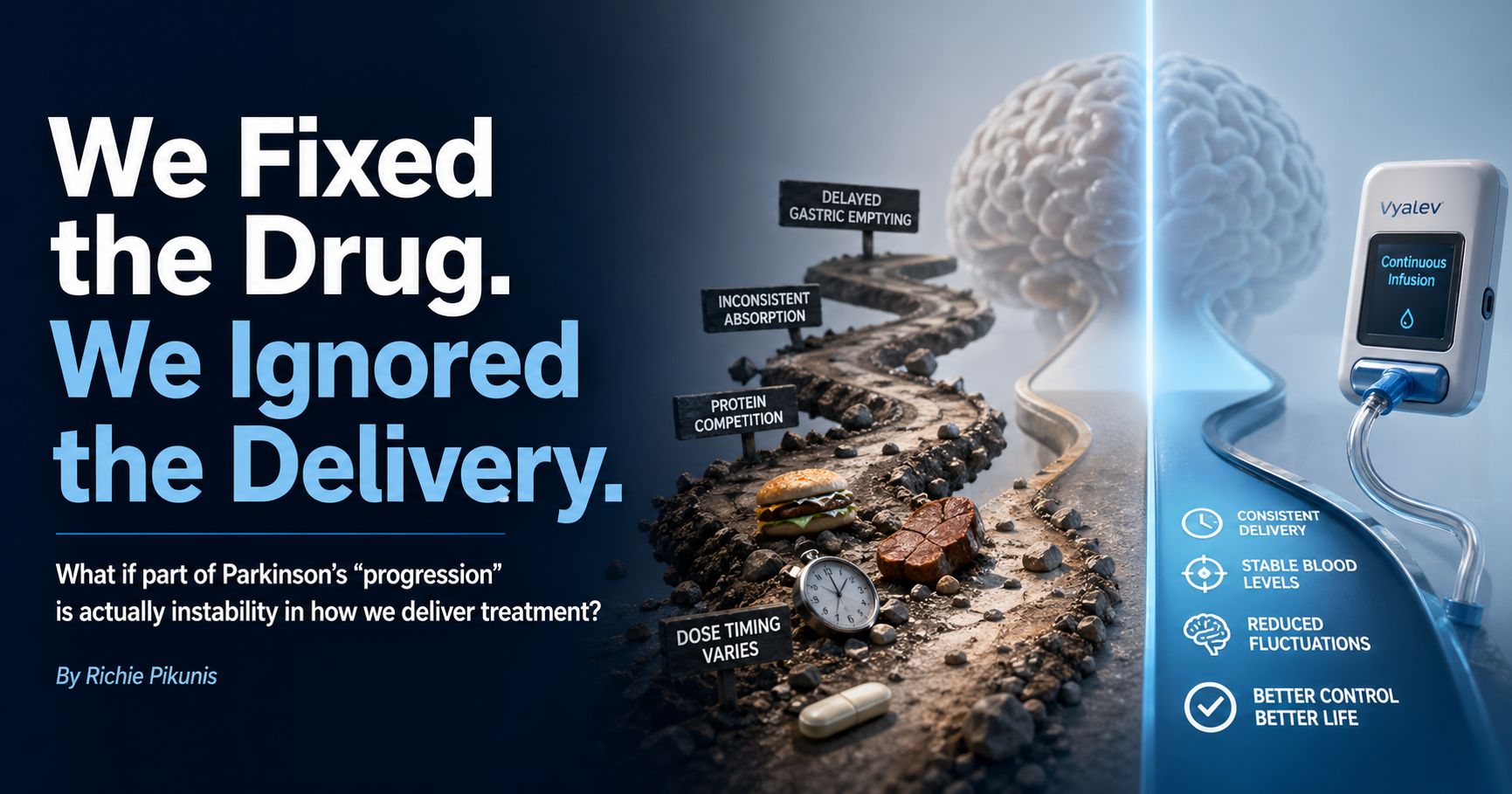
With oral therapy, that means:
delayed gastric emptying
inconsistent intestinal absorption
direct competition with dietary protein in the gut
dose timing that rarely matches real life
So by the time levodopa reaches the bloodstream, the signal is already unstable.
Then we add competition at the blood-brain barrier on top of that and treat the whole outcome as if it is purely disease driven.
But it is not just biology.
It is the system we built around the biology.
What Changes Over Time
Early in Parkinson’s, the brain can compensate.
It stores dopamine.
Buffers fluctuations.
Smooths things out.
Later, it cannot.
That buffering capacity fades, and the brain becomes dependent on real time dopamine levels.
That is when consistency starts to matter more than anything.
And that is exactly when the system we are using becomes the least consistent.
What Changed for Me
I transitioned off oral medication and onto continuous infusion with Vyalev.
Over time, I was also able to turn off my deep brain stimulation.
The blood-brain barrier did not change.
Levodopa still has to compete to get in.
Protein did not suddenly stop mattering.
But everything leading up to that point did change.
No gastric timing issues.
No absorption guessing.
No chasing doses throughout the day.
What was left was a more stable signal arriving at the same biological barrier that had always been there.
And the difference was not subtle.
The Question That Does Not Go Away
If the biology at the blood-brain barrier has not changed,
but the variability has,
what does that say about where the real problem is?
I am not suggesting Parkinson’s is not progressive.
I am asking whether we are underestimating how much of that progression is shaped by instability in how we deliver treatment.
Because when the brain loses its ability to buffer dopamine, variability stops being an inconvenience.
It becomes the problem.
Where This Leaves Us
Protein timing still matters.
The blood-brain barrier still matters.
The biology still matters.
But the delivery system matters too.
And maybe more than we have been willing to acknowledge.
If stabilizing everything before the barrier can change the experience this much in some cases,
that is not noise.
That is something worth paying attention to.
For Clinicians and Researchers
I would value perspectives from those working in movement disorders, pharmacokinetics, and advanced Parkinson’s care.
Specifically around how delivery variability is being accounted for in long term outcomes, and whether we may be attributing more to disease progression than to the systems surrounding treatment delivery.
---